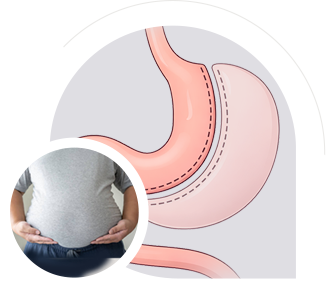
The Sleeve Gastrectomy, also commonly referred to simply as the Sleeve or stomach stapling, is the most commonly performed weight loss procedure worldwide, testimony to its effectiveness and excellent safety.
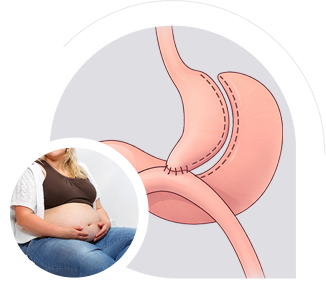
The One Anastomosis Gastric Bypass also known as the OAGB or Mini bypass is a newer, highly effective type of gastric bypass that retains the effectiveness of the original Roux-Y bypass but with fewer side effects. A/Prof Taylor is a world leader in this type of bypass.
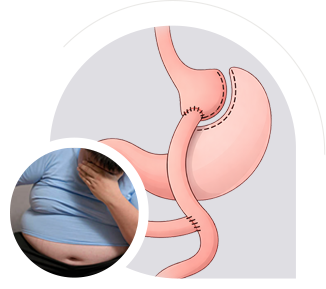
With over 50 years of proven results, the Roux-en-Y gastric bypass sets the standard for weight loss surgery. Although newer procedures have largely replaced the Roux-Y, it still remains the preferred option for patients with severe reflux, including Barrett’s oesophagus.
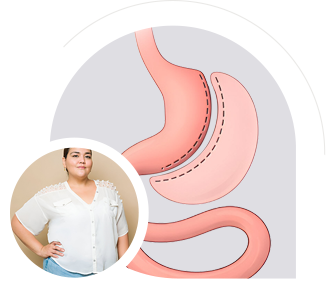
The SADI procedure provides powerful metabolic effect, making it suitable for patients with diabetes or a very high BMI. Because it has a lower risk of marginal ulcers, it is the procedure of choice for patients who smoke or regularly use anti-inflammatory pain relief.
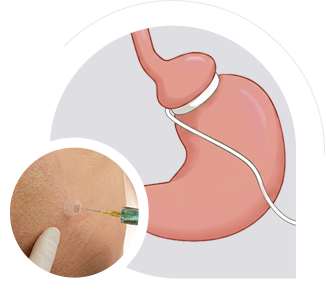
If you already have a gastric band, we also perform adjustments (adding or removing fluid) to optimise restriction or correct reflux and regurgitation. We also perform band removals, either as a standalone procedure or as part of conversion to another form of bariatric surgery (see revisional surgery section)
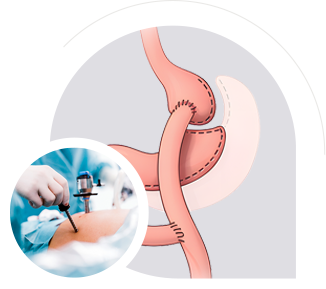
Weight regain can occur after successful surgery due to the lifelong genetic and biological nature of obesity. A/Prof Taylor specialises in revisional surgery to tighten or modify existing procedures, restoring restriction, portion control, and enhancing the metabolic effect to help you regain control.
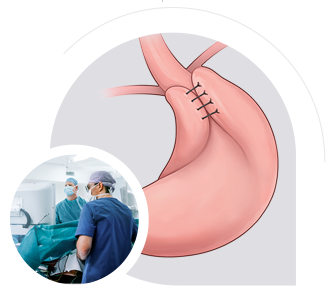
Corrective Bariatric Surgery focuses on resolving anatomical or functional issues following prior weight loss surgery. This may include correcting reflux, regurgitation, swallowing problems, or malabsorption concerns. The goal is to overcome unwanted side effects whilst maintaining effective weight control.